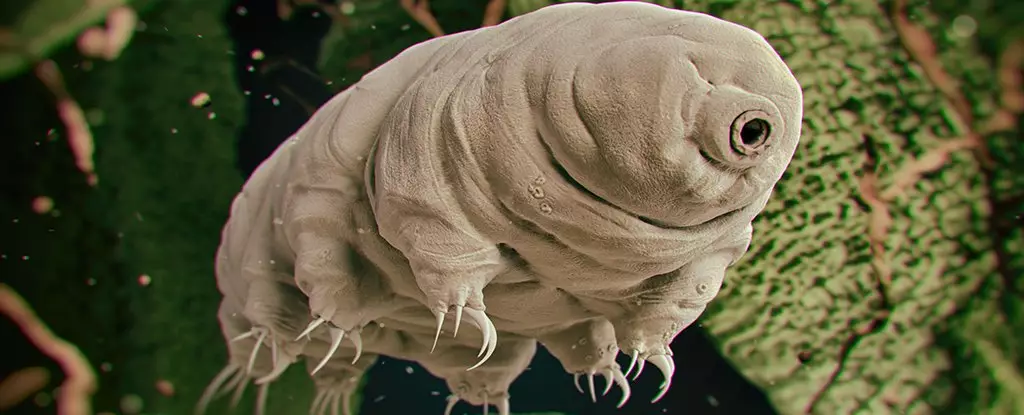
The microscopic marvel known as the tardigrade, often referred to as a “water bear,” is a living testament to resilience in the face of extreme adversity. These tiny creatures can survive environments that would decimate most life forms, including intense radiation, extreme temperatures, and extreme pressures. Recent research has revealed that the genetic secrets behind their extraordinary endurance could provide critical innovations in medical science, specifically for cancer treatment. A groundbreaking study led by Ameya Kirtane from Harvard Medical School and Jianling Bi from the University of Iowa has taken the first steps towards translating the tardigrade’s superpower into practical applications.
Tardigrades possess an astounding ability to withstand lethal doses of radiation—up to a thousand times more than what would be fatal for humans. This remarkable durability is largely attributed to a specific protein called Dsup, short for “damage suppressing.” Discovered in 2016, Dsup has shown promise in laboratory settings for its ability to protect human cells from DNA damage induced by radiation exposure. The implications of this discovery for cancer therapy are profound, given that while radiotherapy targets malignant cells, it also wreaks havoc on healthy tissue, leading to painful side effects and severe complications.
When subjected to radiation, healthy cells can suffer from DNA breaks that not only lead to cell death but also trigger inflammation. Common side effects of radiation, such as mouth sores and digestive issues, significantly impact the quality of life for cancer patients. According to Dr. James Byrnes, a radiation oncologist at the University of Iowa, the effects of radiation can range from minor discomfort to life-threatening emergencies, underscoring the need for protective interventions during cancer treatment.
In their study, Kirtane and Bi’s research team isolated Dsup in the form of messenger RNA (mRNA), which can be injected into human cells. Unlike traditional methods that integrate therapeutic genes into a cell’s DNA, which can pose risks of complications or mutations, delivering mRNA allows for temporary expression of the protective protein, minimizing safety concerns associated with genetic modifications. This approach could revolutionize the way that cancer treatments are delivered, providing a cleaner and more controlled method of protecting healthy cells during challenging therapies.
The researchers took an innovative approach by encasing the mRNA in polymer-lipid nanoparticles designed specifically to deliver the therapeutic agent to targeted cells. This method successfully transported the mRNA into lab-grown cells, enabling them to produce a substantial quantity of Dsup before the nanoparticles disintegrated. Kirtane noted that this combination of polymers and lipids maximized the efficiency of RNA delivery, creating an effective mechanism for introducing Dsup into cells without directly involving the genetic coding of harmful tumor cells.
To test the efficacy of their mRNA delivery system, the research team conducted experiments on mice, comparing the results of those treated with Dsup-encoding mRNA against control groups exposed to radiation without protection. The findings were promising: the ‘rectal’ group that received Dsup treatment exhibited approximately 50% fewer DNA breaks than the control group, while the ‘mouth’ group demonstrated about 33% fewer DNA breaks. Importantly, the Dsup treatment did not interfere with tumor volume, indicating that it selectively protected healthy tissue without hampering cancer treatment.
Despite the encouraging outcomes, researchers caution that these initial results, obtained from small sample sizes in animal models, may not directly correlate with human responses. Nonetheless, this study lays critical groundwork for further investigation, particularly in the potential application of Dsup mRNA delivery for various clinical scenarios beyond radiotherapy. The authors of the study highlight that the methodology could extend to protecting normal tissues from the adverse effects of chemotherapy, addressing chromosomal instability, and even mitigating genetic predispositions to cancer.
The journey from tardigrade resilience to therapeutic innovations is more than just a curious scientific endeavor; it holds the potential to transform cancer treatment paradigms. By utilizing components from nature, researchers aim to mitigate the painful side effects of radiation therapy while maximizing its effectiveness against tumors. As further studies are initiated to explore and validate these promising findings, the medical community looks forward to a future where the lessons learned from these extraordinary creatures can lead to safer, more effective cancer therapies, offering hope and improved quality of life for patients around the globe.